Symptoms and Diagnosis of Athlete's Foot

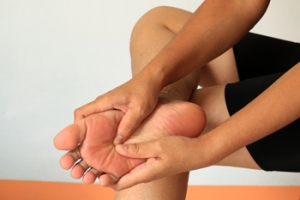
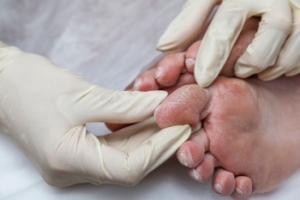
Athlete's foot is a common fungal infection affecting the skin on the feet, particularly between the toes. Symptoms include itching, burning, and stinging sensations, often accompanied by redness, peeling, and cracking skin. The affected areas may also appear swollen and develop blisters. Diagnosis typically involves a physical examination by a podiatrist, who may scrape a small sample of the affected skin to examine under a microscope or send it to a lab for testing. Identifying the presence of fungal elements confirms the diagnosis. Early recognition and treatment of athlete's foot are essential to relieve discomfort and prevent the infection from spreading. Proper hygiene, antifungal medications, and keeping the feet dry and clean are effective measures to manage and prevent athlete's foot. Athlete’s foot can be uncomfortable and unsightly. If you have any of the above symptoms, it is suggested that you consult a podiatrist who can successfully treat this condition, which may include prescribed medication.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Dr. John C. Lawlor from Florida. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact one of our our offices located in Cape Coral and LaBelle, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
See Your Podiatrist Regularly If You Work On Your Feet
Causes of Pain in the Ball of the Foot
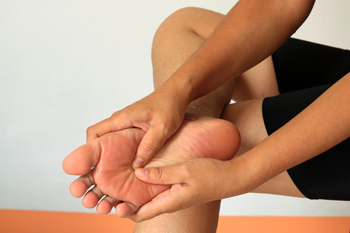
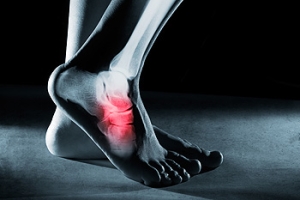
Pain in the ball of the foot, medically referred to as metatarsalgia, can stem from injuries, neuromas, and ill-fitting footwear. Common among athletes and high heel wearers, this pain often results from improper weight distribution across the metatarsal bones. Pain in the ball of the foot also may be the result of Morton’s neuroma, where nerve tissue in the ball of the foot becomes swollen. Foot injuries such as fractures, gout, arthritis, and bunions can also contribute to this metatarsal pain. High heels, in particular, tend to compress the toes and place excessive pressure on the ball of the foot, making matters worse. Persistent pressure or friction from tight shoes can cause calluses that add to the pain. Proper footwear with ample room for the toes and cushioning around the ball of the foot is essential for preventing and managing pain. If you are experiencing pain in the ball of your foot, it is suggested that you make an appointment with a podiatrist for an exam and treatment.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Dr. John C. Lawlor from Florida. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact one of our our offices located in Cape Coral and LaBelle, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
Our feet are arguably the most important parts of our bodies because they are responsible for getting us from place to place. However, we often don’t think about our feet until they begin to hurt. If you have pain in your feet, you need to first determine where on the foot you are experiencing it to get to the root of the problem. The most common areas to feel pain on the foot are the heel and the ankle.
Heel pain is most commonly attributed to a condition called plantar fasciitis. Plantar fasciitis occurs when the plantar fascia, which is the band of tough tissue connecting the heel bone to the toes becomes inflamed. Plantar fasciitis pain is usually worse in the morning, and it tends to go away throughout the day. If you have plantar fasciitis, you should rest your foot and do heel and foot muscles stretches. Wearing shoes with proper arch support and a cushioned sole has also been proven to be beneficial.
Some common symptoms of foot pain are redness, swelling, and stiffness. Foot pain can be dull or sharp depending on its underlying cause. Toe pain can also occur, and it is usually caused by gout, bunions, hammertoes, ingrown toenails, sprains, fractures, and corns.
If you have severe pain in your feet, you should immediately seek assistance from your podiatrist for treatment. Depending on the cause of your pain, your podiatrist may give you a variety of treatment options.
Taking Care of Diabetic Feet
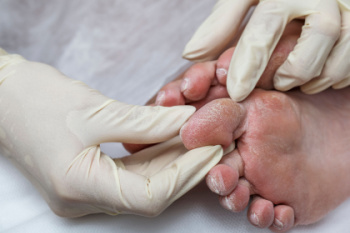 Diabetes is a chronic condition characterized by elevated blood glucose levels due to the body's inability to produce or effectively use insulin. This condition can lead to various complications, particularly affecting the feet. High blood sugar can damage nerves and reduce blood flow, increasing the risk of foot problems. Common issues include neuropathy, which can cause loss of sensation, and peripheral artery disease, leading to poor foot circulation. These complications can result in infections, ulcers, and, in severe cases, amputations if not properly managed. To avoid foot problems, individuals with diabetes should maintain good blood sugar control, inspect their feet daily for cuts, blisters, or changes in skin color, and keep their feet clean and moisturized. Choosing proper footwear is important, as wearing ill-fitting shoes and socks can cause pressure points and sores. If you have diabetes, it is suggested that you see a podiatrist regularly to monitor and manage your foot health.
Diabetes is a chronic condition characterized by elevated blood glucose levels due to the body's inability to produce or effectively use insulin. This condition can lead to various complications, particularly affecting the feet. High blood sugar can damage nerves and reduce blood flow, increasing the risk of foot problems. Common issues include neuropathy, which can cause loss of sensation, and peripheral artery disease, leading to poor foot circulation. These complications can result in infections, ulcers, and, in severe cases, amputations if not properly managed. To avoid foot problems, individuals with diabetes should maintain good blood sugar control, inspect their feet daily for cuts, blisters, or changes in skin color, and keep their feet clean and moisturized. Choosing proper footwear is important, as wearing ill-fitting shoes and socks can cause pressure points and sores. If you have diabetes, it is suggested that you see a podiatrist regularly to monitor and manage your foot health.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. John C. Lawlor from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our our offices located in Cape Coral and LaBelle, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
Definition and Causes of Foot Stress Fractures
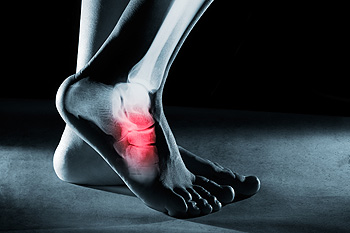
A foot stress fracture is a small crack or severe bruising within a bone, often resulting from repetitive force or overuse rather than a single traumatic event. Common causes include high-impact sports, sudden increases in physical activity, and wearing inadequate footwear. Stress fractures frequently occur in the weight-bearing bones of the foot, such as the metatarsals. Symptoms include pain that worsens with activity and diminishes with rest, swelling, and tenderness at the fracture site. Recovery time for a foot stress fracture typically ranges from six to eight weeks, depending on the severity and adherence to treatment. Proper rest, wearing supportive footwear, and gradually returning to activities are essential for healing. In some cases, immobilization with a boot or crutches may be necessary. If your foot hurts, it is suggested that you visit a podiatrist who can accurately diagnose and treat stress fractures.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Dr. John C. Lawlor from Florida. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact one of our our offices located in Cape Coral and LaBelle, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Stress Fractures of the Foot and Ankle
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
Understanding Different Types of Gout
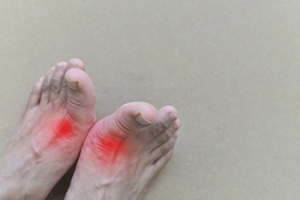
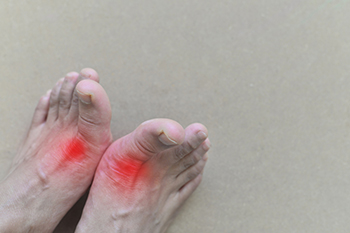 Gout, a form of arthritis, arises from a buildup of uric acid in the bloodstream, causing sharp crystals to form in the joints. It primarily affects the big toe but can also occur in other joints, like the ankle or knee. The uric acid buildup may happen due to certain dietary factors, such as consuming foods like red meat, seafood, and alcohol. Genetics and underlying health conditions such as obesity, high blood pressure, and kidney problems can also increase the risk of developing gout. Gout can present in various forms, including acute attacks, causing sudden and intense pain in the joints. Chronic gout involves recurrent episodes of pain and swelling, which may lead to joint damage over time if not treated properly. Another form, called tophaceous gout, occurs when urate crystals accumulate under the skin, forming lumps or nodules known as tophi. Symptoms of gout typically include severe joint pain, swelling, redness, and warmth in the affected area. If you struggle with gout or any symptoms that may result in gout, it is strongly suggested that you visit a podiatrist to receive proper care and treatment.
Gout, a form of arthritis, arises from a buildup of uric acid in the bloodstream, causing sharp crystals to form in the joints. It primarily affects the big toe but can also occur in other joints, like the ankle or knee. The uric acid buildup may happen due to certain dietary factors, such as consuming foods like red meat, seafood, and alcohol. Genetics and underlying health conditions such as obesity, high blood pressure, and kidney problems can also increase the risk of developing gout. Gout can present in various forms, including acute attacks, causing sudden and intense pain in the joints. Chronic gout involves recurrent episodes of pain and swelling, which may lead to joint damage over time if not treated properly. Another form, called tophaceous gout, occurs when urate crystals accumulate under the skin, forming lumps or nodules known as tophi. Symptoms of gout typically include severe joint pain, swelling, redness, and warmth in the affected area. If you struggle with gout or any symptoms that may result in gout, it is strongly suggested that you visit a podiatrist to receive proper care and treatment.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact Dr. John C. Lawlor from Florida. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact one of our our offices located in Cape Coral and LaBelle, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.